One of the most common conversations I have with patients who have post-paralysis facial synkinesis is this one: “Should I keep doing BOTOX, or is it time to consider surgery?”
The honest answer is that there is no single right answer, and that’s by design. In our practice, we believe this decision belongs to the patient. Our role is to make sure you have accurate information, understand what each path involves, and feel supported no matter which direction you choose.
Our latest research has helped us understand the factors that influence that choice: not to prescribe a path, but to make sure we’re having the right conversation with each patient. At the end, I will always tell you what I would recommend to a family member, taking into account your particular circumstances.
A Note on Timing & Treatment Combinations
Currently, the best results we get are usually a combination of BOTOX and surgery, which act synergistically. If you’ve had synkinesis for more than 16 months, the choice of whether to start with BOTOX or surgery is usually up to you. If you have had synkinesis for less than that period, we usually start with BOTOX.
The following are photos of a patient with Bell’s Palsy who received BOTOX treatments for 9 years before deciding to proceed with surgery. Surgery included selective neurectomies, depressor anguli oris (DAO) myectomy, and platysma myotomy. Photos were taken in January 2015 (15 years after Bell’s Palsy onset) and February 2025 (8 months post-operatively).
BOTOX Treatment
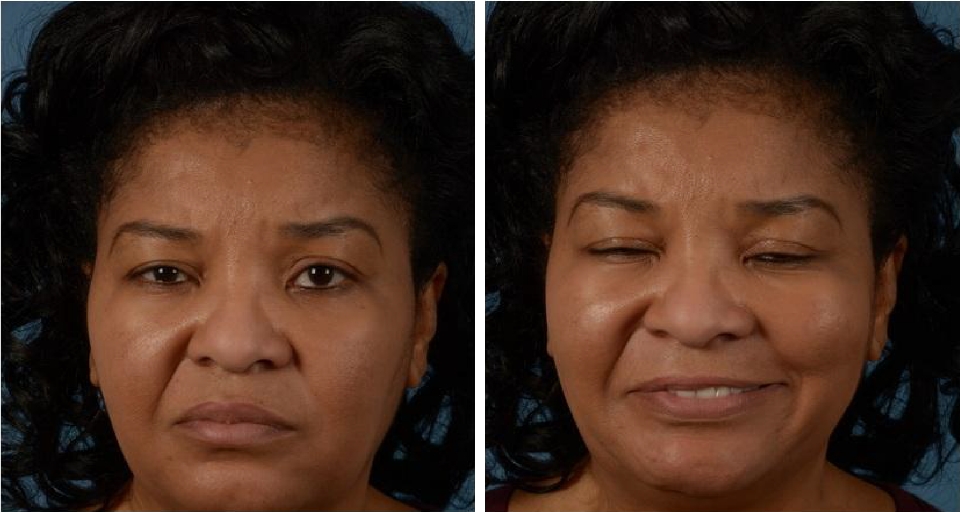
After Surgery
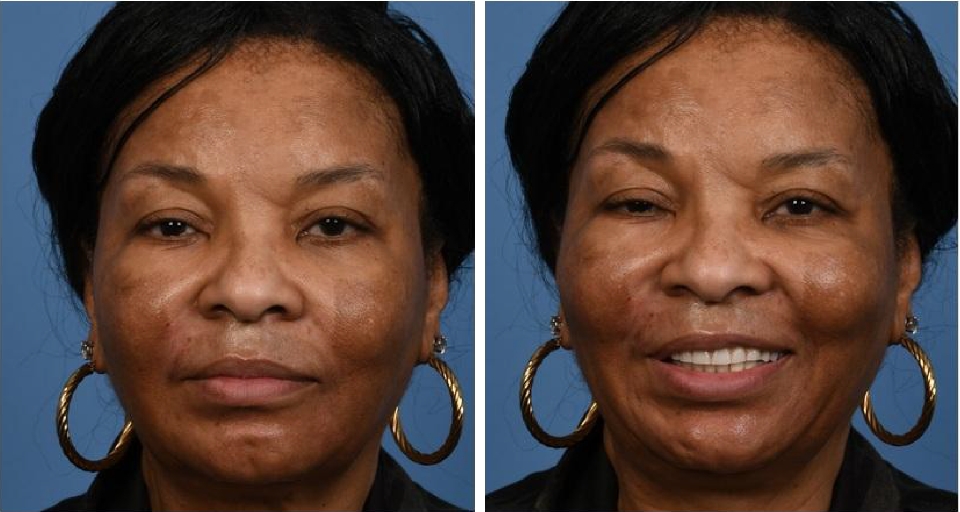
Reproduced with patient permission for medical education. © Shai M. Rozen, MD, FACS.
What the Research Reveals About Treatment Choice
Our study, published in Plastic and Reconstructive Surgery (Bhatia, Rail, Henn, Lee, Rozen; 2025), is the first to examine the patient-related factors that influence treatment selection and timing in post-paralysis facial synkinesis. We reviewed 231 patients treated over a 15-year period (2009–2024) in our practice, comparing those who chose BOTOX alone with those who chose synkinesis surgery. In our practice, synkinesis surgery refers to a combination of selective neurectomies and selective myectomies, with or without BOTOX before or after.
Two factors independently predicted that a patient would choose surgery over BOTOX alone:
Severity of Synkinesis
The first factor was synkinesis severity. Patients with moderate or severe synkinesis were nearly three times more likely to choose surgery than those with mild synkinesis.
This makes intuitive sense. For patients whose symptoms are significantly impacting facial function, appearance, or quality of life—the eye that squints shut when smiling, the neck that tightens when raising the eyebrows, the lower lip that pulls when blinking—a treatment that provides several months of partial relief may feel less satisfying than a more definitive option.
Distance From Our Institution
The second factor was the distance from our institution. Patients who traveled more than 100 miles to see us were more than five times as likely to choose surgery. Nine patients in the study traveled over 1,000 miles, and every one of them chose surgery. This likely reflects a simple reality: if you’ve gone to considerable effort to find a specialist, you may be strongly motivated to pursue the most durable solution available.
Importantly, factors including age, insurance status, socioeconomic vulnerability, how long the patient had lived with synkinesis, and gender were not independently associated with whether a patient chose surgery or BOTOX.
This indicates that the decision is driven primarily by the severity of a patient’s experience and their own goals—not by external circumstances beyond their control.
What BOTOX Offers for Synkinesis & Where It Has Limits
BOTOX remains an excellent and widely used treatment for synkinesis. It works by temporarily relaxing the overactive muscles responsible for involuntary co-movements, reducing facial tightness, and improving overall facial balance. It’s minimally invasive, can be started as soon as synkinesis has stabilized (typically around 16 months after facial nerve injury), and doesn’t close the door on surgery later.
In our study, nearly half of the patients who eventually chose surgery had received BOTOX for an average of 19 months before making that transition. BOTOX is often the first step patients take to understand their synkinesis and what they most want to change, and that experience genuinely informs surgical planning.
For some patients, BOTOX alone provides very satisfying results for years. For others, the cycle of repeated injections every three months—and the return of symptoms if injections are delayed—becomes less acceptable over time, particularly when symptoms are severe.
What Synkinesis Surgery Offers & What It Involves
Selective neurectomies and selective myectomies are targeted surgical procedures designed to address the specific overactive muscles and nerve branches responsible for each patient’s unique pattern of synkinesis. Rather than temporarily quieting overactive muscles, these procedures aim to produce more durable improvements in facial symmetry and movement.
Surgery is more invasive than BOTOX, involves a recovery period, and carries surgical risks. It’s not the right choice for every patient or every degree of synkinesis. In our practice, we don’t offer synkinesis surgery until a patient’s symptoms have stabilized—generally after about 16 months from the onset of facial paralysis—because operating on a face that’s still changing doesn’t make sense.
This is based on our previous study on “The Natural Progression of Synkinesis”, which is discussed in our previous blog post, “The Natural Progression of Synkinesis: What the Latest Research Tells Us”. And we discuss this thoroughly with every patient before any decision is made.
An Important Finding About Treatment Timing
Our study also looked at how long it took patients to move from a synkinesis diagnosis to their first surgery. Two findings here deserve attention:
- Female patients waited, on average, about 441 days longer than male patients before proceeding with surgery.
- Non-White patients waited approximately 355 days longer than White patients.
These are real and meaningful differences, and they matter to us.
We don’t believe these gaps reflect patients making the wrong choice or taking too long. Surgical decisions are personal and complex. Risk tolerance, family responsibilities, insurance navigation, and the time needed to build trust in a surgeon and a care team are all legitimate parts of this process.
What these findings tell us is that we should be paying closer attention: making sure that every patient who might benefit from discussing surgery actually has that conversation fully and without barriers, and that we are addressing any practical obstacles directly.
An Important Finding About Treatment Timing
Both BOTOX and surgery are legitimate, evidence-based treatments for post-paralysis facial synkinesis. Neither is universally correct. Neither is universally wrong.
The research from our program confirms what we see in the clinic every day: the most important factors in this decision are the extent to which synkinesis affects your life and your personal goals—not your age, your insurance, or how long you have had it.
What we ask of every patient is simply this: come in, have the conversation, and let us make sure you have the information you need to make the right decision for you. Whether that path leads to BOTOX, surgery, or a combination of both—we’re here for all of it.
The full study—“BOTOX® versus Surgery: Evaluating Patient Treatment Choices for Post-Paralysis Facial Synkinesis”—is published in Plastic and Reconstructive Surgery and is available at DOI: 10.1097/PRS.0000000000012476 (abstract on PubMed).
— Dr. Shai M. Rozen
Board Certified Plastic Surgeon
Professor and Vice-Chair of Plastic Surgery, University of Texas Southwestern Medical Center


Leave a Reply